The Gout Without Hyperuricemia case study gives us insight into the true nature of uric acid in the real world.
Medical science is driven by statistical analysis, clinical trials, and case studies. Statistics identify potential relationships that can be tested in clinical trials. Real-world case studies then identify exceptions, which may help us refine our understanding, or force us to rewrite the rulebook.
This case study helps us understand hyperuricemia better, and underlines the need to diagnose gout on an individual basis.
Gout Without Hyperuricemia Case Study
This case study is part of my exploration of the nature of hyperuricemia. The definition of hyperuricemia is quite vague, namely:
An abnormally high level of uric acid in the blood.
The definition fails to be definitive, as it depends entirely on the establishment of a “normal uric acid level.”
Though it is perfectly feasible to calculate a statistical norm, the medical value of doing so is zero. For medical purposes, comparison to a norm might give a general indication where to start looking, but it should never be seen as a rule. Many factors affect the transition from hyperuricemia to gout.
This case study focuses on temperature as a major factor that influences that transition. This is my layman’s summary of the published case study:
- Title:
- Gout without hyperuricemia.
- Author:
- McCarty DJ.
- Published:
- JAMA 1994;271:302-3.
The study is published in JAMA without the usual Methods, Results, Conclusions format, and so I will retain the published layout.
It opens with a paragraph explaining that acute gouty arthritis is rare when uric acid levels are consistently normal. However, the case study that follows illustrates the dangers of ruling out gout when uric acid is not high. The case study will explain why the properties of uric acid account for this phenomenon of normal urate causing gout.
Gout Without Hyperuricemia Case Study Report
I have extracted the history of the case as a timeline, so that you can see the progression. It is the study of an 88-year-old man, who by July 15 1992 was wheelchair-bound. I have retained the same units of measure for uric acid, so if you are more familiar with mmol/L, simply add a decimal point. Thus 208 μmol/L becomes 0.208 mmol/L, though we would normally round this to 0.21 mmol/L.
- July 15 1980
- Gout presumed by an internist. Treated with Non-Steroidal Anti-Inflammatory Drugs (NSAIDs).
- July 22 1980
- Uric acid tested at 375 μmol/L (6.3 mg/dL). No test of joint fluid for uric acid crystals
- July 3 1984
- Uric acid tested at 345 μmol/L (5.8 mg/dL)
- 1989
- Uric acid tested at 291, 369, and 357 μmol/L (4.9, 6.2, and 6.0 mg/dL).
- 1990
- Uric acid tested at 387 μmol/L (6.5 mg/dL).
- 1991
- Uric acid tested at 351 μmol/L (5.2 mg/dL).
- May 7-15 1991
- Hospitalized for polyarthritis. Treated with steroid shot plus prednisone and naproxen pills.
- January 11 1992
- Uric acid tested at 351 μmol/L (5.9 mg/dL).
- April 1992
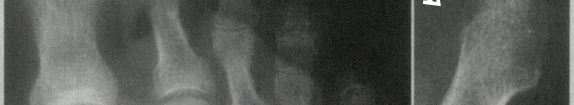
- Right foot painfully swollen and unable to support weight. Codeine for pain control. X-ray shows bone damage [see below].
- May 1992
- Hospitalized for 2 weeks. Various suggested diagnoses, but not gout. Uric acid tested at 291, 363, and 309 μmol/L (4.9, 6.1, 5.2 mg/dL). Treated with naproxen, but only modest improvement at time of discharge.
- July 15 1992
- Start of rheumatologist consultancy. Test of joint fluid reveals uric acid crystals, Patient’s hands and feet cold to touch. Treated with colchicine, naproxen, and ranitidine [presumably to limit side effects of naproxen]. Uric acid tested at 381 μmol/L (6.4 mg/dL).
- July 22 1992
- Foot could bear weight without pain. Uric acid tested at 399 μmol/L (6.7 mg/dL).
Within the case report, the author notes that laboratory test results include a “normal” range. In this case it is 208-506 μmol/L (3.8-8.5 mg/dL). There is also a definition based on the solubility of uric acid, which is explained below. However, the author notes that, whichever definition you choose, all the tests between 1980 and 1992 are considered normal.
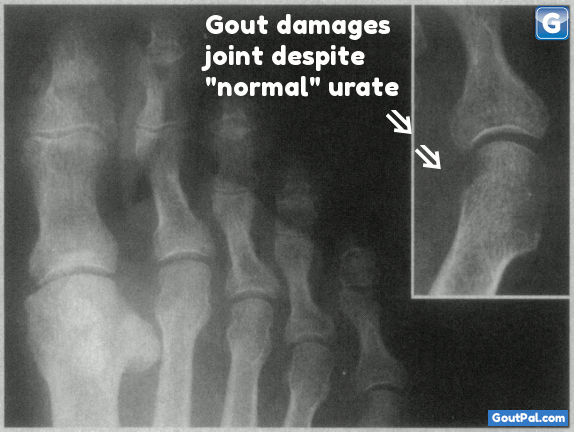
Gout Without Hyperuricemia Case Study Comment
The author starts his commentary with 2 important points about the definition of hyperuricemia:
- What is hyperuricemia, statistically?
- Higher than 2 standard deviations above the mean for a randomly chosen population. Most labs use samples from blood donors [which is almost certain to include some gout sufferers].
- What is hyperuricemia, medically?
- Above the point at which crystals form.
The first definition will vary according to the population sampled [search for Normal Uric Acid? No Thanks! for more information]. The second is generally recognized to class readings above 416 μmol/L (7.0 mg/dL) as hyperuricemia [1]. However that is measured at a temperature of 37 °C. At 30 °C, the crystallization point drops to 268 μmol/L (4.5 mg/dL)[2-3]. Tophi are much more common in colder parts of the body[4], and the author refers to unpublished data that records average temperature of the big toe joint to be 32.8 °C.
Due to this specific case, and the recognition that urate deposits will form more readily at lower temperatures, the author recommends joint fluid analysis (arthrocentesis) in all arthritic patients:
Clearly, arthrocentesis is not an optional procedure in the study of patients with arthritis.
The report concludes with a review of other studies that report gout without hyperuricemia,[5-8] noting that other factors besides temperature must also be considered in individual cases.[9]
Gout Without Hyperuricemia: Next Steps
Hyperuricemia is a strong indicator of gout. However, doctors have long known that high uric acid does not automatically lead to gout. I explain why in my asymptomatic hyperuricemia pages.
Now we can see that absence of hyperuricemia should not rule out gout. Elsewhere, I have explained lower uric acid test results during a gout flare. Here we see that, if gout is suspected but uric acid levels are not high, we must also check other factors. Temperature can have a major influence, and other factors may also affect an individual.
Are you in a situation where you suspect gout, but cannot get a clear diagnosis, because you do not have hyperuricemia? Shout out in the gout forum, and I’ll help you convince your doctors, as I had to convince mine. Lowering uric acid is only relevant on an individual case basis. Statistical, and even medical, generalizations can be a guide, but target uric acid levels must be tailored to the gout patient.
Leave Gout Without Hyperuricemia to browse the Hyperuricemia guidelines
Gout Without Hyperuricemia Related Topics
Please remember: to find more related pages that are relevant to you, use the search box near the top of every page.
Common Terms: crystal, Hyperuricemia, Most Helpful Gout Pages, Urate Deposits
Other posts that include these terms:
- High Alkaline Foods for Gout Diet Menu
- Gout Foods Table for Vegetables
- Gout Food List for GoutPal Foodies
- Foods High in Uric Acid Chart
- Purine Rich Foods
- Does Alcohol Affect Gout?
- Colchicine For Gout
- What Foods Cause Gout?
Gout Without Hyperuricemia References
- Levinson DJ, Becker MA. Clinical gout and the pathogenesis of hyperuricemia. In: McCarty DJ, Koopman WJ, eds. Arthritis and Allied Conditions. 12th ed. Philadelphia, Pa: Lea & Febiger; 1993:1773-1805.
- Loeb JN. The influence of temperature on the solubility of monosodium urate. Arthritis Rheum. 1972;15:189-192.
- Seegmiller JE. The acute attack of gouty arthritis. Arthritis Rheum. 1965;8:714-723.
- Macfarlane DG, Dieppe PA. Diuretic-induced gout in elderly women. Br J Rheumatol. 1985;24: 155-157.
- Hadler NM, Franck WA, Bress NM, Robinson DR. Acute polyarticular gout. Am J Med. 1974;56: 715-719.
- Hall AP, Barry PE, Dawber TR, McNamara M. Epidemiology of gout and hyperuricemia: a longterm population study. Am J Med. 1967;42:27-37.
- Wyngaarden JB, Kelley WN. Gout. In: Stanbury JB, Fredrickson DS, Wyngaarden JB, Goldstein JL, Brown MS, eds. The Metabolic Basis of Inherited Disease. 5th ed. New York, NY: McGraw-Hill International Book Co; 1983:1043-1114.
- Rodnan GP. The pathogenesis of aldermanic gout: procatarctic role of fluctuations in serum urate concentrations provoked by feast or alcohol. Clin Res. 1980;28:359A.
- McCarty DJ. Precipitation and deposition of monosodium urate monohydrate crystals. In: Gresser U, Zollner N, eds. Urate Deposition in Man and Its Clinical Consequences. Berlin, Germany: Springer Verlag; 1991:12-23.
Please give your feedback
Did this page help you? If yes, please consider a small donation. Your donations help keep GoutPal's gout support services free for everyone.
If not, please tell me how I can improve it to help you more.
- YouTube
- The gout forums.