Keith’s GoutPal Story 2020 › Forums › Please Help My Gout! › Looking for gout advice – lots of questions
- This topic has 13 replies, 5 voices, and was last updated 12 years, 1 month ago by
zip2play.
-
AuthorPosts
-
September 25, 2008 at 6:45 pm #3029
fredwilson
ParticipantHi all,
Sorry this is going to be a long message but I want to completely explain my circumstances.
I believe I have had gout for quite a while (years) and never took medicine for it and never got a positive diagnosis from a doctor. I started having “gout” attacks more often and was having them about once every 2 months. Usually I could feel an attack coming on and I could drink lots of water and it would stop the attack. Finally, about 4 months ago my doctor was concerned because my uric acid level was 8.
He told me to start taking 100 mg of allopurinol once a day. Then, if I tolerated it, go up to 100 mg twice a day. I didn’t have any problems with the allopurinol but was still having problems with the gout attacks. He told me to take 300 mg twice a day. I had been taking that amount for the past 3 months when I had a follow-up appointment about 4 weeks ago. He changed my allopurinol to 150 mg twice a day, ordered a blood test, and wanted me to return for a follow-up in 3 weeks. So, I did what he said, had a blood test done 4 days afterwards. The following Monday I woke up to a major gout attack in my ankle and knee. This was 2 weeks ago yesterday and I still can’t put any pressure on my leg. I tried colchicine, indocin, water, etc… nothing really helped. I was taking 800 mg ibuprofen 4 times a day and that made the pain tolerable.
Another follow-up appointment to my doctor 4 days ago. Then he gave me Prednisone, told me to stop taking the allopurinol during the gout attack, and wants me to restart at 200 mg twice a day after I’ve been pain free for 10 days. I asked about my current uric acid reading and it was just over 4. Now from what I’ve read, since I’ve been on allopurinol for 3 months, I should NOT stop the drug during a gout attack.
Now, I’m also having some other issues that I believe may be caused by me taking allopurinol. I have noticed that I am getting “man boobs” and a Google search says that breast enlargement in men is a very rare side effect of allopurinol. I brought this to my docs attention, and he didn’t think it was caused by the drug and sent me for an ultrasound and mammogram. I’m waiting for those results.
My questions are below…
1) My blood test showed a uric acid level of 4. This was 4 days after my doctor lowered my daily allopurinol. Would this be an accurate reading based on the lower amount of allopurinol in such a short time?
2) Would lowering my allopurinol cause this current gout attack even though my uric acid was 4?
3) Do I keep taking my allopurinol during this current gout attack?
4) Should I stay on 150 mg twice daily or go up to 200 mg twice daily (allopurinol)?
5) Has anyone else heard about allopurinol causing breast enlargement in men?
6) I’m a little concerned that my doctor isn’t very versed in gout treatment, should I seek the advice of a Rheumatologist?
Thanks in advance for any/all responses!
Fred
September 25, 2008 at 6:45 pm #2735Arthur Eyetiss
ParticipantColchicine As A Gout Diagnosis Tool
My Dr informed me that gout wears many faces and is different from patient to patient in its onset and symptoms. Initially he took blood to measure uric acid levels to establish a baseline, but readily admitted that the numbers wouldn’t necessarily confirm gout as a diagnosis. The blood-work was also used to rule out any infection. Subsequent testing never showed elevated uric acid levels, so after the first few attacks, he stopped testing blood. The Dr. felt that getting relief from suspected gout by using Colchicine was virtually proof positive that the pain and swelling was caused by gout. Other steroidal and non-steroidal medications could have alleviated these symptoms as well, but only gout would have responded favorably to Colchicine.
So in addition to eliminating a painful attack of the gout, Colchicine can be used in diagnosing gout thereby avoiding the need to draw fluids from the inflamed joint.
For most, depending on the dose, Colchicine will cause cramps and diarrhea, but if you can’t use other drugs, or they simply don’t work, Colchicine is a blessing!
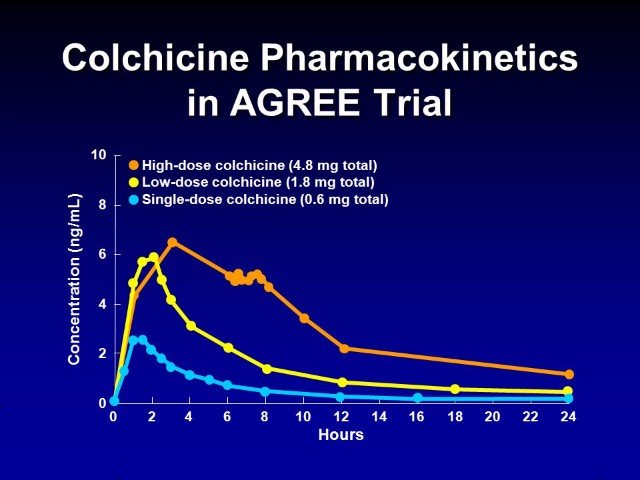
How long does it take for colchicine to work? September 25, 2008 at 7:38 pm #3926Keith Taylor (GoutPal Admin)
ParticipantI can understand the reluctance to draw joint fluid.
To the patient, it sounds painful and intrusive. However, I can assure you, from personal experience, that there is no pain from the procedure. It is very similar to an innoculation, though obviously in reverse.
From the practitioners point of view, it may be an unfamiliar procedure, but if the doctor is unwilling to do it, referral to a rheumatologist is the obvious, and best, answer.
Though colchicine is widely considered to be a gout only pain reliever, PharmGKB lists several other conditions that respond to colchicine.
- [Calcium pyrophosphate deposition disease, acute (prophylaxis and treatment)] Colchicine is used for the symptomatic relief of acute attacks of calcium pyrophosphate deposition disease (chondrocalcinosis articularis; pseudogout; synovitis, crystal-induced). Intravenous administration of the medication is reported to be more consistently effective than oral administration for relief of an acute attack. However, the high risk of toxicity associated with intravenous administration of colchicine must be considered. Prophylactic use of oral colchicine may prevent repeat acute attacks.
- [Arthritis, sarcoid (treatment)] Colchicine is used to relieve acute arthritic symptoms associated with sarcoidosis.
- [Amyloidosis (treatment)] Colchicine is indicated to decrease amyloid deposition and resultant tissue damage in patients with primary amyloidosis or amyloidosis secondary to conditions such as psoriatic arthritis, ankylosing spondylitis, or familial Mediterranean fever. Colchicine has been used together with melphalan and prednisone for the treatment of primary amyloidosis.
- [Behçet's syndrome (treatment)] Colchicine is used in the treatment of patients with Behçet's syndrome. It relieves or prevents erythema nodosum and arthralgias and may also reduce the frequency or severity of oral and/or genital ulcerations in some patients. However, colchicine does not reduce the frequency or severity of ocular lesions associated with this disease or improve visual acuity in affected patients.
- [Cirrhosis, biliary (treatment)] Colchicine is used in the treatment of primary biliary cirrhosis. Biochemical indicators of disease activity (serum albumin, bilirubin, alkaline phosphatase, cholesterol, and aminotransferases) improve during treatment. Although colchicine may retard the development of fibrosis and hepatic failure in patients with biliary cirrhosis, it does not relieve symptoms, prevent or reverse histological changes characteristic of the disease, or decrease the need for hepatic transplantation. In a few studies colchicine-treated patients survived significantly longer than control patients. Colchicine may provide additional benefit when used concurrently with ursodiol for this indication. However, colchicine clearance is substantially reduced in patients with alcoholic cirrhosis. Caution and careful attention to dosage are recommended to prevent accumulation and toxicity if colchicine is administered to these patients.
- [Pericarditis, recurrent (treatment)] Limited data indicate that colchicine may be useful for preventing acute attacks of pericarditis that recur despite treatment with NSAIDs and/or corticosteroids. Colchicine has permitted withdrawal of corticosteroid therapy in some patients with this condition
Of these, clearly pseudogout (Calcium pyrophosphate deposition disease – CPDD) presents a real risk of misdiagnosis. That's not to say your doctor is wrong, just that it's better to be safe than sorry.
February 18, 2009 at 3:59 pm #4117zip2play
ParticipantI am also fond of colchicine as diagnostic. Combined with a couple high uric acid readings I think it is reliable, even considering the possibility of pseudogout.
The worst that can happen is that pseudogout is diagnosed as gout and soon it is shown that allopurinol is useless or uric acid is consistently low even in the face of joint inflammation.
Joint aspirations always have some risk of infection and a joint infection is a medical emergency of the first order and probably more commonly, they have the risk of being done by someone who couldn't find the proverbial polarized dendrite in a haystack. Imagine if every severe joint pain had one's doctor probing for synovial fluid. I, for one would not trust MY doctor to be able to differentiate a crystal of uric acid from one of pyrophosphate under polarized light.
Gout was well diagnosed in times BEFORE the invention of the microscope or before Dr. Land discovered polarized light filters.
March 25, 2009 at 12:59 am #4316Keith Taylor (GoutPal Admin)
ParticipantAfter a two year hiatus I developed gout in my left big toe joint while visiting in another state 12 days ago. Since my last attack two years ago had been mild I decided to ride this one out. Four days later gout developed also in my right big toe joint. Within a few hours I was at an Immediate Care. Since I am on Coumadin the doctor prescribed Colchicine and said it helps with the new onset of gout but that it would not have a dramatic affect on a condition four days old. He was right. Within two days the newly developed case was well on its way out. The older case was getting a lot better but it was clear it had a ways to go. It's now a week after I took the medicine and the worse affected foot is still not entirely back to normal. I am walking on the outside edge of that foot and can't yet put a lot of pressure on the joint. It's a little better every day. This was my third case of gout. The first was seven years ago (Vioxx helped a lot with that one). I think I'm going to have to pay attention now, research, and take some action in regard to exercise, diet, etc. , and what meds won't conflict with Coumadin, Metoprolol, Plavix, Creston, Aspirin. So far I have not run into any mention of these meds conflicting with gout meds in discussions of gout treatments.
Am back home now and wondering if I should go to my regular doctor. The attack is virtually over and I don't know what he could do for me.
March 25, 2009 at 8:41 am #4318Keith Taylor (GoutPal Admin)
ParticipantFred said:
Am back home now and wondering if I should go to my regular doctor. The attack is virtually over and I don't know what he could do for me.
He can monitor your uric acid. It is crucial if you want to control your gout in future to get uric acid out of your system.
Please go and get a uric acid test – be sure to get the numbers, because some labs report the result normal when it is way too high for a gout sufferer.
See what your doc advises, then come back to the forum and discuss it.
March 25, 2009 at 12:10 pm #4321Keith Taylor (GoutPal Admin)
ParticipantThanks for the reply. I'll do that.
I have lots of blood work panel results for the past two years and wonder if uric acid is included in these panels. I'll have to look them over and see if there is any listing for uric acid. I have gone over each one of them as they came in to see what levels are above or below norm. I don't recall any levels ourside of norm for anything called “uric acid”. My outside-of-norm levels were for calcium which ran consistently between 10 and 11, which is higher than it should be. This was being monitored for hyperparathyroidism.
October 20, 2009 at 12:55 am #6149Utubelite
ParticipantI am not an expert but from what ever I know, your treatment sounds very different. I am really surprised that you were taking 300 mg of Allopurinol twice a day ( that is 600 mg daily) wihtout any Uric Acid blood test for 3 months. Generally, the dose is started at 100 mg and then increased weekly with UA tests till time the level drops to target of below 6 ( or 5, 4 etc. whatever the target is).
The Allopurinol should not be started during a gout attack but if the gout attack happens while one is taking Allopurinol, it should be continued.
And now the doctor wants you to stop Allopurinol and then re-start with a dose of 400 mg daily( again too high). I have not heard such a treatment on this forum before.
I do now know what the experts like Zip or Trev or GP feel; If I were you, I will change the doctor asap.
October 20, 2009 at 4:40 am #6150trev
ParticipantWell ,UTube- No expert but certainly a fair share of gout over the years.
In some ways the pulling together of different background experience of 'the many' is an antidote to the well intentioned, but sometimes inadequate, ministrations of the medical world.
It has to be stated again- the legal responsibilty for health advice is with ones medical advisor- but that only goes as far as 'reasonable care' and stops short of 'side effects' responsibilties. These fall somewhere between the courtroom and the unspoken masses who 'do the meds'!
I would say- it takes time to get results, things are still settling down. Freds' attack isn't out of place as we all know (though I don't take AP)- and side effects usually recede on dose change.
Fred: It does seem like the your Dr. is on the case, even if a bit heavy on the doses- Zip would probably find his approach in your case as 'far too uncommon'. Very proactive, I would say- and trying to tread a difficult path on treatment for you!
The reason why 3 attacks seems the threshold for starting uriscoric drugs is exactly because the side effects are often more trouble than the illness. This is true of many drugs in specific cases.
So what I'm saying is: Bear with it a while- you're on track for a handle on your gout and getting tests to clear worries of side effects. Your UA is good- it will need time to pay off and flares are inevitable to some degree- your case rather bad ones.
Docs will rarely admit to side effects- as they can't be proven without a barrage of tests which are worse than stopping the offending drug.
Further they have no wish to cause harm- and therefore bound to be in denial.
They are caught between the grip of the law/procedure and big Pharma.
Stay strong, stick with medical advice – and in a week, I bet things will look better!
October 20, 2009 at 4:46 am #6151zip2play
ParticipantFred,
(I would normally have tried using your post and putting my comments in line by line but I'm afraid our primitive little bulletin board might make a mish-mosh so I;ll do what I can.)
Firstly, your doctor is making a pig's breakfast of prescribing allopurinol. Almost nobody goes to a 600 mg,/day dosage without a LOT of care, certainly not in any kind of quick progression of 100, 200, 600 over a matter of a couple weeks. Once allopurinol is started it is NOT to be stopped during an attack and thrashing around to this super-high dosage and then pulling you off is malpractice. A logical treatment is something like 300 mg/day FOREVER with MAYBE an adjustment every year. Frequent dose changes are going to cause more attacks than prevent.
Gynectomastia (man boobs): I am not an expert here but I think the likely cause, if they have come on recently, is the STEROID treatment, presumably prednisone? that you are taking. The drug of choice for an acute gout attack causing inability to walk is COLCHICINE, taken during one day at a dosage of 2 pills and then followed up by one an hour for 11 more hours…15 if necessary or until exctreme diahrrhea or pain relief intervenes. Do this in ONE day and don;t take more than 2 or 4 pills the next day if you are satill in pain. THe diarrhea can be quite vicuious. Diddling with one or two pills a day during an acute attack is useless.
If you take the colchicine the right way, there is no heed for the huge doses of ibuprofen (I'm amazed you still have a stomach!
 ) Do NOT take aspirin except for a 75 mg/day regimen if you take it for your heart.
) Do NOT take aspirin except for a 75 mg/day regimen if you take it for your heart.1. and 2. There is no need to take a divided dose of allopurinol, its metabolites stay active for several days so taking one dose a day of 300 mg. is precisely equal to taking 2 x 150 mg. Yes, huge doses of allopurinol will bring blood levels down to 4.0 very quickly…alas that sometimes frees up stored uric acid from joints to revisit other sites and cause further grief.
3. Do not stop the allopurinol during a gout attack. The rule is don't START during one, but NEVER wstop.
4. Take 300 mg. allopurinol in a single dose…that's enough.
5. No man-boobs that I;ve heard about from allopurinol. Are you a body builder on any OTHER anabolics?
6. Your doctor IS trying but he sounds out of his league here and is thrashing around with try thi-try that. See aa rheumatologist.
Addendum: Have you had the classic TOE? Are YOU certain of the gout diagnosis (never mind the doctor.) Remember colchicine is somewaht diagnostic. If it doesn;t work in the BIG dose, then let the rheumatologist make a final determination…perhaps with a joint fluid bioply during an attack.
Re-addendum: You might be amazed at how rapidly you can abort the worst attack with colchicine done right.
WHEW!
 October 20, 2009 at 6:48 am #6159
October 20, 2009 at 6:48 am #6159fredwilson
ParticipantFirst off, thanks to everyone for the quick responses!! Now some more info and a plan that I'll need comments on.
As I suspected, my doctor seems to be going a bit crazy on the allopurinol. I think I'm going to take the 300mg ONCE a day instead of 150mg twice a day for now until I can go see a rheumatologist.
The gynecomastia didn't show until I started taking the allopurinol. That's what led me to research if it's a side effect of the drug. The prednisone was only started 4 days ago and is only being taken for a week. I'm not a weight builder, in fact, I weighed 375lbs about 2 months ago and have started working to get my weight down. I'm now down to 350….hmmm, could weight loss be a cause of my gout flare up?
I have used colchicine before and it always kicked the gout out in a matter of hours if I took it early enough. I find that I can usually get to just over 4mg in 6 hours before the diarrhea kicks in. I have also read that taking a small, daily dose of colchicine during the initial start of allopurinol helps keep the gout attacks away while the body cleanses itself.
In regards to this current gout attack I'm having, it's now just about gone. I don't have the constant pain but I can't put full weight on my leg and my knee is still swollen, I can't bend it much more than 45 degrees. From my past experiences, I'll be ok in a few days. That being said, I tried the heavy dose of colchicine on the SECOND day of my current attack and it didn't do a thing.
Yes, I have had the classic “toe” on both feet. I've also had attacks in both feet, knees, and in my right elbow this past Memorial day. Speaking of my elbow… I've had problems in the past couple of years being able to straighten it out. Never thought much of it but since being on the allopurinol this seems to have resolved somewhat. Could this be from the cleansing of the joints due to the allopurinol?
So, how does this plan sound?
1) Continue 300mg allopurinol ONCE a day.
2) Go see a rheumatologist.
Hmmmm…. I guess that's it. LOL
Thanks again!
October 20, 2009 at 7:46 am #6160trev
ParticipantFred- You don't give your location or age, which would help a bit on this.
What stands out is your weight and recent losing of it.
Losing more than 2lbs a week ,as you are, is not usually recommended- though it is commendable in effort terms.
The loss of weight is going to add to the effects of AP- so you will be accelerating your UA residue clearance some. Hopefully you are now finding a reasonable balance.
Reducing your weight , over an extended period will help your joint pain, if caused by overwear.
There's no reason why you can't have multiple causes- gout is just more attention grabbing, as we know!
You probably have arthritis in your family, too!
I think your 'plan' is sound- *add something about long term weight loss goals-and stick to it. [2lbs/week max!]
This will reduce stress on joints and lower need for SUA reducers to stay any higher than you want.
October 20, 2009 at 9:00 am #6161fredwilson
ParticipantTrev,
I'm in the U.S. and I'm 41.
As for the weight loss…. Yes, I totally agree with you in regards to how much/often. I originally lost quite a bit when I started and I believe it was due to mostly water weight. I am trying to stay on the 2-3lbs per week schedule but I have only been doing this by doing the Weight Watchers program. My plan was/is to start exercising when I physically can (gout attack gone). I'll have to really keep an eye on my weight and eating so I don't start to lose too much too fast.
I just have to keep telling myself that I didn't get to this point in months!
October 20, 2009 at 2:52 pm #6163zip2play
ParticipantFred,
Losing the 25 pounds rapidly could have , let me get the word right, “emptied” some of the fat out of your pecs leaving saggy skin that is giving the IMPRESSION of breast tissue. Real gynectomastia can be boobs on a skinny man and then be very easy to diagnose as probably hormonal. For someone 350-375 I think it might be just illusion…just a little sag.
Yes losing weight fast liberates a lot of nucleic acids whose only route out of the body is conversion to uric acid. Continue the weightloss but know that you now have allopurinol blocking some of this conversion. I hope with further loss your man boobs but into hard pecs at 200-250 pounds with some serious bodybuilding…never too late to start.
So if youve had both TOES, then you definitely have gout but whether your current knee bout is due to gout or something else is hard to tell…knees are funny. With non response to colchicine maybe not gout. Elbow might be more likely.
But your steady treatment with 300 mg allopurinol and a visit to your rheumatologist is precisely correct. Test your uric acid again and if you see another 4 you are sliding into home free.
-
AuthorPosts
- You must be logged in to reply to this topic.