Stopping Gout Together › Forums › Help My Gout! The Gout Forum › First gout attack, wondering do I need meds
Tagged: Allopurinol Drug Forum, Forum for Gout Victims, Most Helpful Gout Forum, Normal Uric Acid Forum, Should I Walk with Gout Forum, Uric Acid Blood Tests, Uric Acid Crystals Forum
- This topic has 17 replies, 4 voices, and was last updated 2 years, 8 months ago by
nobody.
-
AuthorPosts
-
-
June 14, 2020 at 5:03 pm #9828
 Pi4aParticipant
Pi4aParticipant
Got my first gout attack about 8 weeks ago – my left thumb was swollen and painful and was not able to move it. Took ibuprofen and next day was more or less ok. Now 8 weeks later the thumb is still a bit painful and it and it gets worse when walking longer distances.
Got to doctor several weeks later when COVID-19 restrictions was a bit reduced. Blood tests where ok (Uric acid 402 (270-470)). But x-ray showed “initial signs of osteoarthritis”.
After rheumatologist visit got diagnosis “gout, gouty arthritis” – confirmed by USG (some tophi around the joint and some more findings specific for gout) and suggestion regarding diets, checking Uric acid levels every 3 moths and take some meds in case of acute flare-up. But no Uric acid lowering meds as it is in range now and start thinking about it in case, if levels go way out of range.After that checked my old labs and I have had raised uric acid levels (540) once more than 4 years ago and have done several tests later where levels bumped around 440-450 mark, that’s near the top of my labs range (470).
Now I’m wondering, should I ask my GP for allopurinol, as I have some tophi + already some findings in x-ray or stay with advice regarding diets and hope that tophi will resolve with time without meds. Any advice would be appreciated.
-
June 14, 2020 at 7:24 pm #9829
nobody
ParticipantHi!
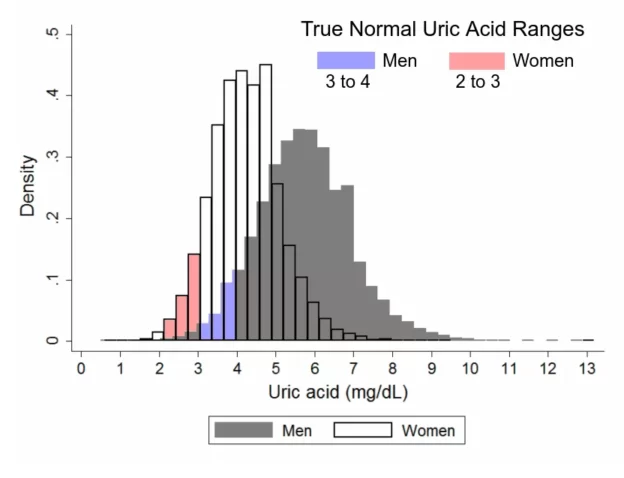
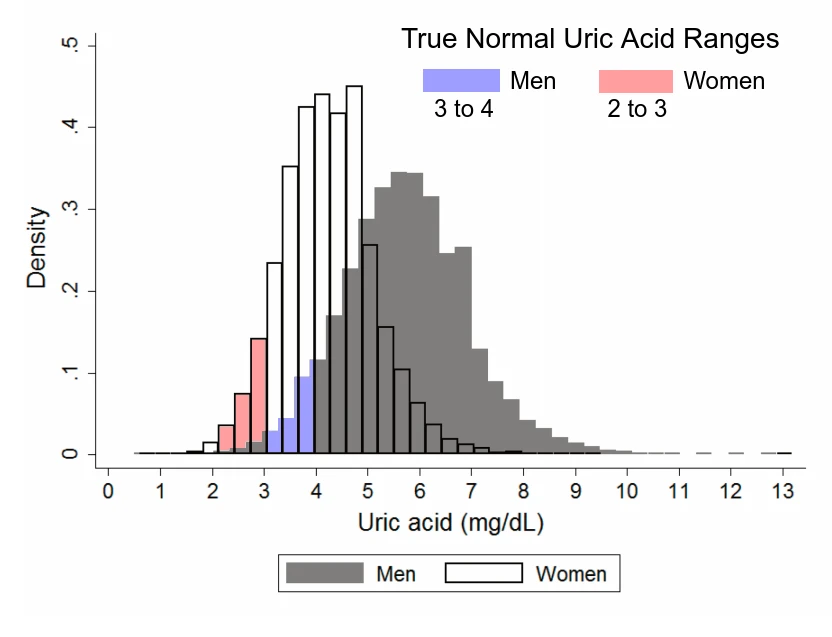
402 is well outside of the range you want your uric acid to be in. That’s definitely not OK. If it was, you wouldn’t need to do anything about your diet, would you? Nor would you have gout. So forget about your lab’s range. It’s not even supposed to be relevant in treating gout.
The problem with UA lowering meds is that they have dangerous side effects. So you could start by trying to fix your uric acid problem with diet. But unless you used to have an alcohol problem or your diet used to be crazy bad, chances are you’ll end up on UA lowering meds anyway and some of the damage done by allowing the disease to progress in the meantime can’t be undone afterwards. This is in any case no emergency so you can afford to take your sweet time working with your doctor to make sure allopurinol is safe for you to take. You could also try very low doses at first, getting your doctor to check your liver function and stuff before taking potentially dangerous amounts. Doctors unfortunately often reason that since there’s no emergency, they might as well do nothing until your health has deteriorated so much that it unquestionably justifies the use of a potentially dangerous drug…
If you are going to try dieting, one problem is that the recommendations are typically useless. We can go over that if you want but allopurinol works so much better than diet that you might not want to bother. -
June 29, 2020 at 6:38 am #9837
 Pi4aParticipant
Pi4aParticipantThank you Nobody. I’m also wondering regarding possibility to lower my uric acid levels with diets alone, as my diet is more or less ok at the moment and I doubt, that I will see needed impact to my UA levels with diet changes alone.
But I’m wondering regarding excess weight. I’m 1.85 m (6ft 1in) tall and wight approx 101 kg (222 lb) at the moment. I have lost some 5 kilos in last several moths with adding daily exercises and some adjustments to my diet, but it’s all before I run in to gout flare up. I’m continuing with exercises (with some changes as jogging/running/walking stuff is a bit painful) and I’m wondering, how large could be weight loss impact to UA levels. -
June 29, 2020 at 2:07 pm #9838
nobody
ParticipantWeight loss and exercise can raise uric acid but what matters are the effects in the long run, and you’ll have to be patient and monitor any benefits with repeated testing over the coming years.
It’s definitely not as simple as a linear relationship between weight and uric acid. Your weight loss maintenance diet matters of course but there may also be weight thresholds. The effects may take a long time to appear as well because your metabolism requires time to adapt. Your diet may also change over time after losing weight, if you had pathological weight-induced insulin resistance for instance.
My guess would be that if you had no symptoms of metabolic syndrome, it’s the diet which matters rather than weight as such.Long story short: in most cases, allopurinol is more effective and works much faster than weight loss.
-
June 29, 2020 at 6:50 pm #9839
 Pi4aParticipant
Pi4aParticipantMy goal is to start with allopurinol to get uric acid levels below 300 and continue with exercises and diet improvements. I have GP appointment in few days and will ask for prescription for allopurinol, but as my uric acid levels are below labs max range (still to high for gout) and has been there for last 4 years, I doubt the my doc will agree to this. So I’m digging thru this forum and other internet sources for second option without uric acid lowering drugs.
-
June 29, 2020 at 7:26 pm #9841
nobody
ParticipantThere are many drugs which reduce uric acid, some of which might be more appropriate if you have other health problems.
But if your doctor doesn’t want to give you any drugs and you can’t see another, we can at that point go over all you could do in terms of diet… which is probably more than you think (but more inconvenient as well!). Some foods even work a bit like drugs, except you can’t control the dose properly. -
July 31, 2020 at 4:17 am #9984
Malik A.
ParticipantHi all,
I am very interested in learning more about the side effects of these drugs, allopurinol in particular. I have been battling an attack for 3 weeks now (day 22). I was taking Colchicine and naproxen together, but it was upsetting my stomach, so the doctor switched me to Colchicine and prednisone. On my latest labs, they discovered that my liver values were elevated. I have never had issues with my liver values before, so the doctor reasoned that the Colchicine is the culprit. So, I have stopped taking it. However, she said once the attack subsides, she wants me to start taking allopurinol. But after searching around some (including some of the posts I’ve read here on the forum), it seems allopurinol can also affect the liver. So, now I am terrified of starting it. It’s an awful fix to be in: gout and what comes with that on one hand and viscous side effects of the medications on the other. I should add that I have been on a plant-based diet for years now. So, I don’t know what else I can do diet or lifestyle-wise to keep my UA numbers under control. (My latest UA results were 6.8.) So, I wanted to ask the good people on the forum for ideas and advice. What do you suggest regarding allopurinol, keeping my liver numbers in mind? And does anyone know if colchicine and allopurinol cause permanent damage to the liver or is this perhaps reversible?
-
July 31, 2020 at 9:53 am #9990
nobody
ParticipantHi Malik,
I didn’t want to barge in your discussion with Keith who has his own process.
But one thing that’s too often neglected about drugs is dosage. Nowhere in your posts do I see a dose. But I’m sure you understand both the effects and side effects of drugs depends on dosage! Even doctors neglect this issue sometimes and stick to whatever dose is printed on a box because they simply don’t have time to understand how to dose every drug.A low dose of allopurinol is quite effective and every additional milligram has a decreasing effect. Some of its side effects can be a problem at any effective dose but if you don’t get any of the serious ones and only have to live with the mild side effect on liver function, that’s highly (and non-linearly) dependent on the dose you take.
For different reasons, medical guidelines recommend you start with a low dose of allopurinol (such as 50 mg) anyway and increase it progressively if you experience no bad reaction and after blood tests show that you’re doing OK. If you did that patiently (something some doctors have little patience for unfortunately), you’d learn what dose your liver can tolerate.
If you were to get a bad reaction from allopurinol, there are alternatives (febuxostat in particular, which works the same way and has the same dosage issues).
So there’s no reason to be “terrified” by allopurinol. If you have East Asian ancestry, a genetic test might be advisable however (depending on the result, it would be prudent to take febuxostat instead).As you might have guessed, taking enough indo, naproxen, colchicine and so forth is key if you want to stop an attack. Taking one pill is often not enough. But of course side effects can also become a problem as one increases the dose…
Note that stomach discomfort on anti-inflammatories is commonly adressed by taking them with another class of drug called PPIs.
All these drugs can disturb your liver.Posting your actual liver function numbers (old and recent) might shed some light on the situation because I don’t know if your numbers are barely above the norm (which is quite common, and doesn’t seem to disturb doctors) or seriously elevated. It might also be helpful if you told us if you have any history of liver problems or had imaging revealing how much fat there is in your liver (failing that, your BMI and age would be informative).
As to your diet and lifestyle, there are things you can do but I wouldn’t recommend it as an alternative to allopurinol. Instead you could try such changes in combination with a lower dose than you might have needed otherwise.
People who eat only plants (and micro-organisms or mushrooms) apparently tend to have elevated uric acid. This is probably because on the on hand, many protein-rich (and especially lysine-rich) foods contain compounds which elevate uric acid and on the other, dairy contains a compound which lowers uric acid. While abstaining from animal flesh is a simple way to lower uric acid, abstaining from dairy and eggs (the main protein sources which do not elevate uric acid) is problematic.
We can discuss these issues in more detail if you want but starting allopurinol (or another drug which lowers uric acid) should be your priority. Attacks can last for months without effective treatment and modern guidelines do not recommend waiting until an attack has susbsided. The only reason to delay treatment would be if another disease mimicking gout is suspected and doctors are waiting for the test. -
July 31, 2020 at 11:23 am #9991
Malik A.
ParticipantHi Nobody,
Thank you so much for responding to my post. I am learning so much on this forum, and the information has been extremely helpful. It also helps to know there are others who understand what you’re going through. As far as dosages, I started by taking 1 Naproxen pill 500 mg and 1 Colchicine pill 0.6 mg daily. As I mentioned, this upset my stomach. So, after four days of that combination, the doctor switched me to a methylprednisolone pack: six tablets the first day, five the second, four the third, three the fourth day, tapering down to one tablet daily. But that had little effect, so she put me back on 1 Colchicine pill 0.6 and started me on 30 mg of prednisone daily. I did the 30 mg of prednisone for 4 days, then 20 mg for 4 days, then 10 mg for 4 days, along with 1 Colchicine pill 0.6 for the 12 days. While this lessened the severity of the attack, it did not “knock it out,” as I read some people said it did for them. I still have quite a bit of swelling in the toe and soreness (pain level is about a 6/10). Also, I noticed the knuckle of my right index finger was swollen and a bit painful as well. I’ve never had that problem before, only in the toe. The doctor seemed perplexed (for lack of a better word), as she said I should not be experiencing a flare up while on prednisone. This of course greatly saddened me. At any rate, after this, the doctor got the blood work back and saw the elevated liver values. In the past they have been within the normal range: 0-44 IU/L. This time, however, it was 87 IU/L. I looked back, and my numbers over the years were 22, 19, 31, 28, 26, etc. nothing over 41 in my history until now. However, I did have an image done about a year ago that showed some fat on the liver. At any rate, she told me to cut back on the colchicine and ordered a new test for a month from now to see if my liver numbers go back down. But my concern is that if I start taking Allopurinol, my numbers will remain elevated. You mentioned that all these drugs can “disturb” the liver. I was wondering if they are known to cause permanent damage or is it reversible after stopping the medication? (I assumed it was reversible since she wanted me to cut back on the colchicine to see if the numbers went back down. Am I right in my assumption?)
As for my age, I am 49. I weigh 160. I have always been on the thinner side (BMI 23.6), and I’m not of East Asian ancestry.
As for the Allopurinol dosage, she wanted me to start with 100 milligrams a day, but only after the attack subsided. As I mentioned, she was against prescribing Allopurinol to me during the flare up. Said it would only make the problem worse. So, I haven’t started it as of yet. She also wants me to continue the prednisone, 10mg a day only for a week to see if that gets it calmed down.
As far as diet, I have read that foods like mushrooms and asparagus can be problematic. I actually started the plant based diet to help with high cholesterol & diabetes. It actually did wonders for me in those areas. I did however read that eggs & dairy are beneficial in the fight against gout. I’m trying to adjust my diet even further to help deal with gout (UA) as well.
With that said, I would love to hear your thoughts on my situation and any other advice or direction you might offer. Thanks again for your assistance.
-
July 31, 2020 at 12:35 pm #9992
nobody
ParticipantYeah, the liver numbers should drop back down after quitting the drug but that can take some time. Allopurinol is permanent however which is why you want to get the dose right.
My guess is that the number you’re talking about is ALT (reference ranges vary across time and place) and that the other liver numbers are OK. If so, 87 isn’t too bad considering the drugs you were taking. Note that the ALT/AST ratio can be informative even if the latter is within the reference range.I can not comment on the prednisone dosage unfortunately but you weren’t taking enough naproxen or colchicine. The colchicine dose you took is at best adequate for prevention or in combination with an anti-inflammatory (traditional dosage to stop an attack is much more aggressive). And stopping a serious attack after you allowed it to start would require a good bit more than 500mg naproxen, colchicine or not. I can not possibly recommend taking more than the maximum recommended dose (even though that might be necessary in some cases) but 500mg is well under half that dose, though there is of course your stomach to consider which means you’d need to either try a coxib instead or take a PPI on top… so I can understand trying prednisone.
There are more exotic drugs to suppress gout symptoms and of course there are always painkillers… suppressing inflammation is best but if you can’t take the stronger doses I’m talking about because of the side-effects, taking a proper painkiller (ask your doctor for the real deal because gout is no joke!) on top is always an option. I’ve had to merely in order to get a couple hours of sleep during an attack.
A small amount of allopurinol every day might seem like something to be avoided but compared with the above, it’s really no big deal. Gout is something you really want to prevent rather than stop once it’s started!About diet, you need to keep your other health issues in mind. Gout is painful but less likely to kill you than diabetes or heart disease. Making your diabetes or cholesterol worse in order to take a bit less allopurinol isn’t worth it. What fats are you currently eating and how is your glucose control?
In theory, both glucose and fat metabolism could affect gout attacks as well. I’ve never seen actionable data about this but it’s something to keep in mind if you experiment with diet. It’s not all that surprising that your doctors are puzzled by your symptoms when your diet isn’t typical. -
July 31, 2020 at 7:33 pm #9994
GC Gopro
ParticipantI am also new to this forum and have made my first post recently. I cannot take any NSAID’s because of any allergy to them. I do not like taking anydrugs unless I have to and am taking allopurinol daily and recently caved in on the colchicine when things got bad, but am off that now.
I have gotten a lot of relief from cold therapy. For years because of my job I had back pain (which is a lot better since I retired from 5 days a week!). The regular use of an ice pack was my go to relief and it worked well.
During my recent and now ended flare, I filled a bowl with cold water enough to cover the foot and emptied a tray of ice in it. I then put a towel on the floor next to the bowl. I sit in the armchair with my foot submerged for some minutes and then extract. The process can be repeated. Do not submerge for too long and monitor how red you skin is, so as you do not overdo it. It takes the heat straight out of the foot and will reduce the inflammation, giving instant relief. Afterwards, you can the raise the foot on a footstool and your organs will not be affected!
I lost a twin brother at age 54 to non-alcoholic fatty liver disease. People often think its all about fat in the diet, but sugar is often a bigger
culprit. It effects the liver like alcohol if the dose is big enough.From what I have read on this disease, if we are willing to be disciplined and take the medication required to reduce the uric acid, I understand you can get rid of gout for good.
-
August 1, 2020 at 11:33 am #9995
Malik A.
ParticipantGl Gopro,
Thank you for your response. It is always helpful to hear from others & to find out what they have done to combat this issue. I am sorry to hear about the loss of your brother. My sincerest condolences to you.
I have also found some success using cold therapy, even if only temporarily. I found that it took down the swelling, which in turn reduced the pain. However, at the height of the attack, this wasn’t enough to give me long term relief. But I still use it faithfully because any relief from this kind of pain is welcome.
I’m glad to hear you are doing better at the present moment. Yesterday (& this morning) are the best days I’ve experienced in 3 weeks. The pain is down significantly, & the swelling is a lot better. The foot is not as warm to the touch either. It’s certainly not back to normal, & I can still feel those twinges, but any relief from that pain is welcome. I will continue using the cold therapy & plan on starting Allopurinol as instructed by the rheumatologist. I’m hoping to get this latest attack completely behind me. The last one was two and a half years ago. I recently invested on a uric acid meter & will monitor my UA levels like I do my sugar. Based on my last A1C results, my sugar is under control well. The problem now is that prednisone causes the sugar to spike significantly, so the sooner I can stop taking that, the better.
As far as the liver issue, I have been researching quite a bit. I will continue to try to keep my sugar in check & add exercise & healthy choices to my lifestyle. Hopefully, that makes a difference.
Here’s to a gout free day.
-
August 11, 2020 at 9:17 am #10029
 Pi4aParticipant
Pi4aParticipantHi all and thanks for good info, Nobody. After GP appointment I started to take Allopurinol 100 mg daily (started from 50 for one week) + dietary changes and exercise and and after bit more than one moth Uric Acid level is down to 295, so will continue to do what I do. So looks that gout is under control. While investigating issues with gout had x-ray for both hips due to some discomfort there and found out, that I have some coxarthrosis in both hips. Doctor does not think so, but I’m wondering, could there be some relation between gout and arthritic changes in hips? As I’m in my late 30s this should not be age related issue as I understand it. Any thoughts would be appreciated.
-
August 11, 2020 at 12:38 pm #10030
Malik A.
ParticipantPi4a,
So happy to hear you got everything under control. I hope everything works out with your hips as well. I am still in the thick of the battle myself. I have the Allopurinol, but as I have mentioned here on the forum, I am concerned because of already elevated liver enzyme numbers. I know the answer is to work this out with a doctor, but it has been next to impossible to get an appointment at the present moment (COVID-19 concerns, I suppose) & the phone tag with the doctor’s office has proven fruitless. I finally have an appointment with my GP this weekend. However, I’m afraid she will pass everything off on the rheumatologist who has not been very helpful at all. I tried to switch rheumatologists yesterday but was told I would be considered a “new patient” & wouldn’t be seen until next year!
Well, anyway, I’m always happy when I read success stories like yours. Gives me hope, & hope right now is golden.
-
August 11, 2020 at 10:09 pm #10031
nobody
ParticipantThe drugs you take for the symptoms aren’t helping your liver either, Malik. The sooner you find a drug that gets your uric acid under control, the less likely you are to end up abusing your liver with other drugs.
The only way to know what allopurinol does to you is to try it, starting with a very small dose and doing enough blood tests to get a good picture of what’s going on (if anything). People sometimes take too much, naturally resulting in liver issues among other problems. Don’t be that careless and you’ll probably be fine. You can’t be your own doctor but you easily be can beat most doctors when it comes to numbers.
The only liver value you posted isn’t alarming (yet). And frankly, this is generally not the main worry with allopurinol. -
August 11, 2020 at 10:16 pm #10032
nobody
Participant@Pi4a: I don’t know how hip problems or imaging work but you’re a little young to have developed gout there. But now that you’ve started a gout treatment, you’ll know soon enough if it cures your hips anyway… let us know in good time what experience will have revealed!
-
August 11, 2020 at 10:32 pm #10033
Malik A.
ParticipantNobody,
So true. Your point is well taken. I will start the Allopurinol at a low dosage to start. You bring another question to mind: how often should one take blood tests to monitor things? This time the doctor (rheumatologist) told me to wait a month to take my next test. Also, how often should one get uric acid tests done? I bought a UA monitor, but I’m not to sure about the accuracy of the results. Overall, the reviews were good. However, several people seemed to complain about fluctuating results. For example, I took it one time & got 11.2. Seconds later a second reading was 4.3 Then 5. So, I don’t put much stock in the monitor.
-
August 12, 2020 at 12:14 am #10034
nobody
ParticipantOne month is reasonable. It’s not ideal but there are costs and even slight risks involved in a proper blood test so you don’t want to overdo it either. If your situation was concerning, you would definitely want more frequent tests but, going by what you told us, I’m actually surprised you were offered a test so soon.
Even if the readings from blood droplets are unreliable (you might get better at it with experience), any extra information is good to have as long as you handle it properly: use averages, calibrate against proper blood test done immediately before or after a droplet test and so forth.
Keep in mind uric acid is nothing like glucose however. Gout is a slow disease. You aren’t a diabetic trying to manage short spikes during the day. High uric acid for a few hours isn’t dangerous so you’re aiming for a safe average (although that target might need to be a bit lower if you get more spikes than most). While testing throughout the day or even every day might be interesting, it’s not necessary to manage gout.
And there are factors like the temperature of your joints, how well-hydrated you are as well as the zealousness of your immune system which affect the level at which uric acid becomes a problem so there’s no absolute number you should aim for in the first place, making precision less useful. This is a learning process and you’ll figure out what values are OK or problematic over time (keeping in mind changes in your lifestyle might require recalibrating your targets). At first, all we can tell is what’s clearly fine, grossly excessive or somewhere in between. Side-effects allowing, best err on the side of safety initially and keep your uric acid quite low.
-
-
AuthorPosts
The forum ‘Help My Gout! The Gout Forum’ is closed to new topics and replies.