Stopping Gout Together › Forums › Help My Gout! The Gout Forum › Hemoglobin, allopurinol, and febuxostat (Adenuric)
Tagged: Adenuric/Febuxostat/Uloric Forum Topics, Allopurinol Problems Solved, Xanthine and Gout Forum
- This topic has 17 replies, 3 voices, and was last updated 5 years, 10 months ago by
d q.
-
AuthorPosts
-
-
May 31, 2017 at 1:42 pm #4006
d q
Participant
Hope your all well guys,
Just a quick update, if you remember my previous dose of 300mgs had me at 336 ummol/l then we moved up to 400mgs. Well the results have come back and UA levels are now at 286 ummol/l. Great news however;
We’ve had a look at my haemoglobin levels snow starting allopurinol and they have been dropping almost with every increase of allopurinol. My rheumatologist said we can try Uloric and gave me a prescription for it.
He said we can do this two ways;
1. Stop allopurinol and start Uloric straightaway and watch what happens. Potentially reducing risk of a gout flare but at the risk of not properly identifying if allopurinol was causing the haemoglobin drop as nothing else has changed with bloods (kidney/liver)2. Stop allopurinol for a month or so to see if the haemoglobin recovers before starting Uloric to confirm if allopurinol was the culprit. If it does return to normal levels then try starting Uloric at the risk of a gout flare in the monthly wait timeframe.
What do you guys think? Could a gout flare occur in just a month of stopping allopurionol..?
I mean we have been at safe levels for over a 2 months now, could that one month interruption while we check haemoglobin levels in 30 days disrupt the recovery procedure and cause a gout attack?
In your experience does Uloric even have a good safety track record..?
Thanks

Can Uloric be halved or quartered?
-
May 31, 2017 at 3:12 pm #4007
nobody
ParticipantI don’t think you know for a fact that your haemoglobin levels “have been dropping almost with every increase of allopurinol” because so far as I know you didn’t test twice at the same allopurinol dose.
Could the problem be dose-independent or possibly unrelated to allopurinol?I’m clueless about this haemoglobin thing so unless your doctor has already looked into every possibility, I would look into the following before changing a medication that works:
-how’s your ferritin doing? could you try an anemia treatment (even if you didn’t change your diet, allopurinol can effect digestion)?
-is there a known link between allopurinol specifically and haemoglobin levels or is it likely related to low uric acid instead (in which case switching medication isn’t likely to help)?
-could you simply try to reduce your allopurinol dose first (you may be past the need for 400mg)?Also, why wait a whole month to test your blood again if the heamoglobin issue is urgent?
If on the other hand it’s not urgent, why not stick to your 400mg allopurinol another month and see what happens?As to Uloric, it’s obviously newer than allopurinol but it’s been on the market for a while now. Have you looked for published studies?
In my opinion, one risk factor with Uloric is not related to the actual drug but to the dosage guidelines. Instead of starting patients on a small dose, doctors often tell them to take roughly the equivalent of your current dose straight away. The businesses enjoying a monopoly on the drug in the US and Europe don’t even sell pills designed to allow for smaller doses (or for slightly larger doses should that be required).
I expect the average Uloric user takes a significantly stronger dose than the average allopurinol user. And if studies showed that Uloric is about as risky as a less powerful allopurinol dose, that would suggest to me Uloric is actually safer. -
May 31, 2017 at 5:12 pm #4008
d q
ParticipantI may have not tested twice but they have been literally in parallel of each other. Even if it was dose independent, its obviously caused some haematological disturbance. All other blood work tests are fine. That includes iron, kidney, liver to name a few. The ferritin and iron saturation levels have in fact gone up slightly because one prognosis is the body has tried to compensate for the lower haemoglobin by trying to absorb more iron from food in order to build haemoglobin up again. Those levels were absolutely fine prior to Allopurinol. The ferritin and iron saturation were going up as the uric acid and haemoglobin was going down.
I’ve done some research (including speaking with rheumatologist) to suggest Allopurinol is in fact linked to a decrease in haemoglobin and potential anaemia. We have these technical articles to refer to:
https://www.drugs.com/sfx/allopurinol-side-effects.html (under hematologic)
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1768933/He wasn’t too comfortable waiting another month to see what happens as he felt almost convinced. Frankly speaking I don’t want to hang around waiting to see if it gets worse. A month is the minimum time recommended before seeing any reasonable change in haemoglobin. So a blood test next week may show a very slight improvement but thats not definite. An upward trend needs to be seen and that would generally take no less then 4-6 weeks.
I agree entirely with the dosage, he wants to put me on 80mgs of Uloric and see how that goes but has left the choice for me to take. So i’m now torn between stopping all treatment for a month with that gout flare risk (if there is one?) or going straight to Uloric and not knowing were we are heading but not risking the gout flare.
Personally, the haemoglobin issue seems a little more concerning as thats been rock solid for literally all my life. Same goes with Liver and kidney.
I’ve done some very basic research on Uloric and blood levels and it seems as if they share very similar side effects “but not everyone gets them”. The major difference is Uloric is metabolised in the liver and Allopurinol in the kidneys. Some swear by it and are relieved to be off allopurinol whereas others found allopurinol better.
Im worried this is going to turn into a toss a coin on which option to try first scenario.
I mean it did take 6 months to go from 580 ummol/l to 283 ummol/l. Can uric acid hit peak levels in a month and strike back with a gout attack or would it generally take a little longer then a month to see any notable change/attacks?
-
May 31, 2017 at 6:15 pm #4009
nobody
ParticipantWhatever you do, do NOT take 80mg Uloric. That’s pointlessly strong and might make your hemoglobin situation much worse.
40mg would likely be more than enough and it would be safer to start even lower.re: “I may have not tested twice but they have been literally in parallel of each other.”
Anything with progressive onset might be in parallel. That’s the problem with not testing twice at the same dose. It would be a strange coincidence if it was unrelated to allopurinol but coincidences occasionally happen.
Sure, anemia is a known side-effect of allopurinol. The thing is, it’s also a known side-effect of Uloric. So is anemia caused by the drugs or by something which both drugs do?
Now if the problem is indeed serious and if there’s little hope of regular anemia treatments working (they’re not only for iron) or of getting a better diagnosis with further testing, I guess trying Uloric makes sense.As to your coin toss, it should come down to what you fear most: gout or this hemoglobin thing.
In my experience uric acid can climb back very quickly indeed if you still have crystals (and my guess is that you do). But I’m pretty sure you’re not going to end up dead because you’ve not taken xanthine inhibitors for one month whereas I’ve got no idea how serious this hemoglobin thing might end up being. -
May 31, 2017 at 8:28 pm #4010
d q
ParticipantAgreed. The haemoglobin is definitely the priority now so I think I’ll turn of allopurinol tomorrow and take blood tests bi-weekly to see how the UA levels and haemoglobin levels pan out. Im not expecting much in the way of a haemoglobin change but I’ll be so upset to see the UA levels rise.
I guess one final option would be to reduce allopurinol to 200mgs and see how that goes but that would put me in gout hell surely? I was at 386 ummol/l on 200mgs of Allopurinol and the rheumatologist mentioned that might be just enough to keep you at bay to see if your haemoglobin recovers to safer levels on that lower dose.I’m really holding onto the wishful thinking that the last 40 days of being on 400mgs and at 283 ummol/l enough crystals have dissolved to keep an attack at bay just for a little longer until we investigate the haemoglobin problem. I’m distraught that its come to this.
Can you believe the UK only dispense 80mgs as the lowest dose.
Could I just not cut the tablet in half and see how it goes myself? -
June 1, 2017 at 6:11 am #4012
nobody
ParticipantI assume that if there are no 40mg pills on offer, it’s because the UK uses Adenuric rather than Uloric. The 80mg Adenuric pills are designed to be easily cut in half.
That would not be quite satisfactory because someone in your situation might for instance want to try 50mg and you’d have a hard time cutting Adenuric pills to such a dose.As to your crystals, I don’t think it’s merely wishful thinking to hope that you might not get an attack right away. What matters is that the stuff that’s been cleaned out of your system isn’t going to build back immediately. So you are now less at risk of a really bad attack than you were earlier.
Lowering your allopurinol dose seems reasonable to me (else I wouldn’t have suggested it) but especially if you’re going to get tested again in 2 weeks, you’re going to get clearer data if you go cold turkey. The allopurinol you already took is going to remain somewhat effective for a few days to begin with. -
June 1, 2017 at 12:47 pm #4026
d q
ParticipantYes, they’re marketed as Adenuric here in the UK. Could I not try 40mg and see how that goes then move up to 80mgs myself if it doesn’t fall within safe limits? At the end of the day it seems we understand more then these gout rheumatologists anyway! Seeing him yesterday made me feel I was talking with an amateur.
I guess the best option would be just to sit tight, quit cold turkey and see if the haemoglobin recovers in the next 4 weeks. If it recovers, we can always try Uloric at 40mgs or even try 200mgs Allopurinol again.
On average how long does it take Allopurinol to clear out of ones system entirely?
Thank you for your vote of confidence nobody. It really does help.
Today was horrible, it felt so strange keeping the meds in the cupboard. -
June 1, 2017 at 1:22 pm #4027
nobody
ParticipantOf course you can experiment with doses but I’m pretty sure 80mg would be way too strong. These are dangerous drugs and some of the side effects seem dose-dependent. Don’t risk it.
Instead, I would rather experiment by starting with less than 40mg (pill-cutting tool required) and seeing what that does.The value of a doctor isn’t that they are a storehouse of information which happens to be obviously revelant to your case but that they know about lots of stuff which is irrelevant to most of their patients but which might just be important to you… stuff it would never occur to you to research.
About the time it takes for allopurinol to be washed out of your system, that may not be the right question because we don’t know what’s messing with your hemoglobin.
My understanding is that allopurinol proper is eliminated quickly but that it’s turned into some other molecule which has a long half-life in the body. Best look it up instead of relying on my recollections!
But that molecule might not be the issue either. It could be some more indirect effect that’s merssing with your hemoglobin level… and who knows how much inertia might be involved? If it’s low UA which is inhibiting hemoglobin production, that should recover quickly but if for instance some alteration to your bone marrow is involved, your hemoglobin could possibly keep dropping for a long time. Like I said, I’m clueless about this.
If testing in 2 weeks seems too short, what about 3? 4 seems kind of complacent if you’re not taking any xanthine inhibitor in the meantime. -
June 2, 2017 at 6:07 pm #4031
d q
Participantperfect, i’ll take a look around for some pill cutters. Worst case scenario is we can always just cut it in half to start with and work downwards or upwards. Like you say, we don’t want to overload the body too much as side effects are real.
Doctors wise, I also agree, they are not necessarily the books in the library but more so the librarians. They know were the books are and have a pretty good idea of how to reference them if they need to or assist someone if they need to.
I’ll do a little research as to how long allopurinol generally stays in the body but my opinion I think as you say its not long. You see the kidneys are responsible for producing EPO which is a hormone that stimulates bone marrow to create blood (which in turn increases haemoglobin). If Allopurinol as a chemical leaves the body swiftly and since Allopurinol is metabolised in the kidney then the kidneys should ideally return to their optimal functional level (correct EPO levels for my condition) regardless of the duration of whatever molecules are floating around UNLESS, those molecules are indeed what is causing the blood haemoglobin suppression.
We have become speculative specialists 🙂
Finally, I saw my GP today to discuss this briefly with her and she asked me to do a blood test today so we have a baseline a day after stopping. She went on to say we will do one in two weeks and then a further one two weeks later. She really is extremely supportive and wants to get to the bottom of this just as much as I do.
I guess the coin has been tossed, Allopurinol has stopped, and now its about the consequences (if any) over the next 30 days.
Wish me luck nobody.
-
June 3, 2017 at 6:26 am #4037
 Keith TaylorParticipant
Keith TaylorParticipantSorry for arriving late, d_q. I thought this was just a general chat and I was waiting for some spare time. Anyway, I’ve changed the title and moved it here from General Discussion.
I’m concerned about a few points. But, I need to go more research on hemoglobin and gout before I can say much meaningful. In particular, I’m in the dark about what constitutes a safe hemoglobin level. Because I’ve been bitten badly by normal values related to uric acid.
I can see that male values should normally be between 130 and 180 g/L. But, safe levels are harder to determine. So far, I’ve seen one report that suggests 120 is not a real concern. In the hemoglobin and allopurinol report, the data shows higher levels than that. Also, hemoglobin appears to rise again after 3 months.
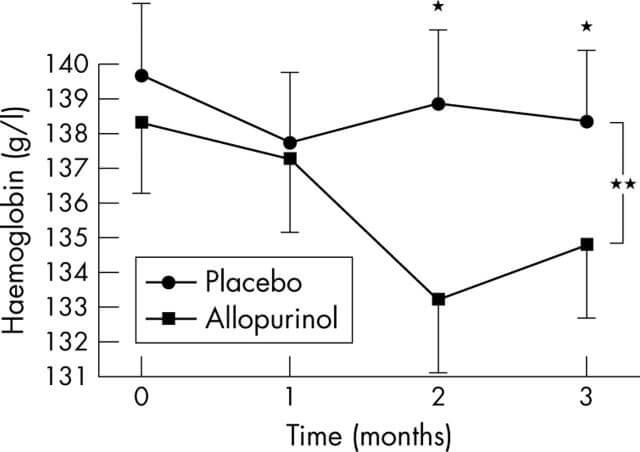
What level of hemoglobin is safe?
So question one is: is your hemoglobin a real issue? Or a temporary blip?
I.e. what hemoglobin history have you got?
Obviously, if you are in danger of anemia, you have to take action. But, I’m concerned that if this is only a short-term issue, with little consequence, you risk throwing out the baby with the bathwater.As for Adenuric, I also can’t locate 40mg in England. But, I saw a hint that Scotland has it (so far unconfirmed). The main problem reported with febuxostat relates to liver problems. But, if you get liver function tests, alongside uric acid tests, it is quite easy to monitor this.

Is Adenuric 40mg (febuxostat) available in UK?
-
June 3, 2017 at 10:16 pm #4042
d q
ParticipantHi Keith, yep, I started the thread in the general discussion forum because I thought it was more of a friendly catchup between us usuals on my situation 🙂
Anyway, if its more appropriate here the thats also fine.With regards to haemoglobin and safe levels, if you remember a few months ago I was a little worried to start Allopurinol because of my thalassemia and how it may affect the condition, well my haemoglobin generally lies around 7.5 – 8.0. Now any human can tolerate a few g/dl up and a few g/dl down. The problem in my case is that it has dropped by about 2 points to 5.5g/dl. I don’t have any specific symptoms (yet) as my body generally is accustomed since birth but it has led my haematologist to be a little concerned going forward. We discussed a number of options in connection with the change of lifestyle after starting allopurinol like increased vinegar intake, water intake, cherry intake, etc. and none of them seem to be indicators for g/dl decrease.
We then moved onto pharmacology factors like my incredibly long gout attack (that is still linguering around), naproxen usage, if any colchicine was used, etc. and we couldn’t find any link.
Finally we looked at Allopurinol and we noticed a steady decline of haemoglobin approximately 3 months after starting it (in December). The decline was almost linear with Allopurinol so we’ve decided to stop it cold turkey to see if it will reverse the drop.
You have experience with starting and stopping Allopurinol Keith, do you think one month without Allopurinol might trigger a flare? I’ve been on it since December and my uric acid has been about 283 ummol/l for all of May and around 336 ummol/l for around all of April.
Any pointers or direction you can give generally too?
Thanks mate.
p.s. thank you for that graph. It is indeed interesting.
-
June 4, 2017 at 6:15 am #4043
 Keith TaylorParticipant
Keith TaylorParticipantGeneral discussion is for non-gout. How’s your family? Where’s this year’s holiday (vacation)? What does the Donald mean to you? That sort of thing.
But this topic is seriously gouty.
Anyway, I can’t remember the medical history of every member. So, I forgot about your thalassemia. Sorry, d_q! My immediate suggestion is (but see my last paragraph first):
1. Get a pill cutter (UK Amazon link that will earn me about 5p if you use the link. So, don’t worry if you have a different source)
2. Start febuxostat as soon as pill-cutter arrives.
3. After 2-4 weeks get a uric acid blood test and the usual kidney function and liver function tests.I realize it can be worrying to think about potential liver effects of febuxostat. But, it’s a rare occurrence. Medicine for complex cases is challenging. But, we’re lucky to live in an age with different options.
Finally, reading between the lines, am I right in thinking you are off allopurinol at the moment, d_q? If so, it might be a very good idea to get a 24-hour uric acid excretion test. Because, if your uric acid excretion rate is low, it can often be fixed with probenecid.
-
June 4, 2017 at 8:20 am #4056
nobody
ParticipantAs far as I can tell, the liver effects of febuxostat are actually quite common. Is there anyone reading this who has taken febuxostat without getting a markedly depressed AST/ALT ratio?
The issue is, are the effects bad enough to warrant discontinuing the drug? Usually that is not the case. But the more you take, the worse the effects are likely to be. Hence pill cutting.
Note that you can cut the Adenuric half-pills with a sharp knife. It’s not very practical (the fragments are likely to fly away from the pressure required to cut the pill) but it works. And you need no tools or preparation to break the pills neatly in half.
Also note that some pill cutters do not work well with Adenuric pills.About the excretion test, my rheuma says you need weeks without meds to get a clean result.
But then DQ was planning to stay off the meds for a few weeks anyway. If my hemoglobin was at 55, I would probably want to see the value recover a bit before trying another drug which is known to cause anemia. -
June 4, 2017 at 5:21 pm #4071
d q
Participant@Keith, no worries mate, like I said it was because I didn’t want to clutter this forum with the usual team’s technical exhaustive discussions.
anyway; yep, I stopped allopurinol on the 1st June and did a blood test the very next day to baseline everything. I’m going to hold off both the allopurinol and febuxostat until I get tested again in mid June and again during the first week of July. If the haemoglobin shows any signs of recovery (even just an upward trend) then I’ll give febuxostat a shot. Since they both work in the same way except where they are metabolised it would probably be safer for things to settle down and allow all medication to leave the system first before starting anything again. It could be nothing to do with allopurinol but we will soon find out. Mid-way through June when I see my GP again I will be sure to bring up the 24 hour UA excretion test. How does that work?
@nobody; yes, i’m a little concerned about the level of attention the liver abnormalities side effect gets. I guess the usual health vs benefit lingo comes into play here. Assuming allopurinol was the culprit I will be sure to start with 40mgs febuxostat and not 80mgs as my rheumatologist suggested.
Yes, 55 is pretty low and it would probably be wise to sit and wait for a month or so. Just out of curiosity, will the remaining half of the pill still be of use? It won’t for example oxidise and lose its effective properties (out of wrapper and cut in half)?Keith, out of curiosity, when you stopped Allopurinol did you get an attack shortly after? That is my biggest concern! I’m constantly worrying that an attack may strike as the levels of UA increase over the next few weeks.
nobody, I know your going to say summon the powers and patience to press on for the next 25 days and I will.. 🙂
-
June 6, 2017 at 2:35 pm #4114
nobody
ParticipantI don’t know whether any effectiveness is lost by cutting the pill but I doubt the effect (if any) is significant. Not that it would matter as we can’t predict precisely how effective a specific dose of the drug would be to begin with. You’ll have to judge the effectiveness of the treatment based on blood tests and/or symptoms anyway.
Just stick to a consistent pill-cutting routine.
-
-
June 6, 2017 at 11:30 pm #4119
d q
Participant@nobody; agreed on the dosage situation. I’ve got my second blood test next week and a visit to the haematologist to discuss and check things out. Since stopping allopurinol every time I get a touch of pain in either of my feet I think it’s a gout flare about to start. Yes, I’m that worried. I really don’t want to take any drugs at least until my first blood test next week. Around 23 days or so to go until the end. I bet my uric acid levels are already at 400 ummol or something. Type something to keep up my morale 🙂
@Keith; I was wondering if you had a chance to read the above post #4071.Finally and off topic, the known UA lowering tomato and gazpacho soup aside, are eating lots of tomatoes in general ok with uric acid (purines etc.) or would it be wise to limit them for now despite them being fruit/vegetable purines..?
Thanks
-
June 7, 2017 at 7:52 am #4120
 Keith TaylorParticipant
Keith TaylorParticipantd_q, there’s lots of gouty topics here that are very interesting. So, if I miss a point or two, just give me a mention. Or start a separate topic.
24-hour urine test
Simply collect your pee for a day as a special gift for your doctor. The lab measures the amount of uric acid you excrete. If it is low, uricosuric drugs or food will improve excretion rates. Then that should lower uric acid. Personally, I think it should be law for this test to be taken if uric acid lowering therapy is not straightforward. Check the manifestos, d_q, and vote accordingly tomorrow.Stopping uric acid lowering therapy
3.5 years, and no gout attack. But my case is completely different because I got rid of almost all my uric acid crystals except for the deeply entrenched ones. Your situation is very different d_q. Because you are only a few weeks (days?) into gout recovery. So, that recovery process is on hold. But, that’s a good thing if it leads to a better long-term plan.If you get a flare, it happens. Don’t overthink it.
Pill cutting
Will you leave the second half of your pill in the garden? Birds might sneeze on it. Cats might piss on it. Rain might make it soggy. My best advice is: pop it back in the packet. It will remain perfectly ready to do its job next day.Tomatoes and gout
I’ve been told off anonymously for my tomatoes advice. Because I’ve failed to mention some recent science (even bad science is still science). I’m still mulling over my response because it’s complicated. You can promote the urgency by starting new topics on tomatoes and gout every day.Happy Christmas
I just thought I’d add something to try and make this the longest thread ever! 😉 😀Too frivolous? Sorry, but there might be some serious points. Also, who will be first to claim the prize for spotting the missing “sh”?
-
June 9, 2017 at 8:02 pm #4125
d q
Participantoh you are an interesting character;
24 hour test; I’ve got that on the list to mention to her next time (GP), also got it on the list to mention to the new rheumatologist in july.
uric acid medicine stop; I was on allopurinol from December until May 31st 🙂
The lowest reading I got to before stoping was 283 ummol/l for around 40 days and 336 before that for about 4 weeks, and 386 for the remaining period.. so I’ve had a good 40 days of intense clearing and another 90 odd days of mild debulking. Nowhere near as much as you but hopefully it will be enough for a little longer until we see were things are heading.pill cutting; haha! cheers mate, good to know.
tomatoes; thats a little scary, I eat loads of tomatoes, does the research provided warrant reduction in consumption levels generally? actually, don’t worry I’ll start a separate thread..!
Happy Christmas; lets enjoy summer first 🙂
-
-
AuthorPosts
The forum ‘Help My Gout! The Gout Forum’ is closed to new topics and replies.