Stopping Gout Together › Forums › Help My Gout! The Gout Forum › Probenecid Questions – How Probenecid Helps Gout
Tagged: Allopurinol Problems Solved, Baking Soda for Gout Forum, Colchicine Problems Solved, Forum for Gout Patients, Gouty Tophi Forum, Prednisone For Gout Forum, Uric Acid Blood Tests, Uric Acid Control
- This topic has 17 replies, 4 voices, and was last updated 6 years, 1 month ago by
 Keith Taylor.
Keith Taylor.
-
AuthorPosts
-
-
January 10, 2016 at 6:21 am #2695
Gout Patient
Participant
My husband is a long time gout sufferer. He is 47, was diagnosed at age 27. He has hyperuricemia, levels of uric acid fluctuate between 8.2 and 8.3 most times he is checked. His flares are increasing both in intensity and duration; he has been nursing a current flare with residual pain for about 1 month. He has over the years tried allopurinol and Uloric; the Uloric gave him heart palpitations and he did not like the way allopurinol made him feel, so he discontinued use against doctors wishes. He takes indomethacin as needed for gout, but his doctor finally persuaded him to try probenecid with a colchicine prescription as well. He has a history of noncompliance with medication. He hasn’t had a test to determine if he is an over-producer or under-excreter. But due to his refusal to take allopurinol, I guess it didn’t matter to the doctor.
I have some questions regarding probenecid. Is it safe for him to take any indomethacin while on the probenecid? Does he take the colchicine only during flares? I read to drink baking soda water while on the probenecid, how much should he take of the baking soda? Is probenecid safer or more dangerous than allopurinol?
He is in constant gout mode and it hurts me to see him in such pain. I am hopeful the probenecid helps but if it starts to make the old crystals flare I am concerned he will get spooked and stop, even though he needs to get the UA levels way down.
Any advice or information is appreciated.
-
January 10, 2016 at 6:21 am #769
Anonymous
Inactive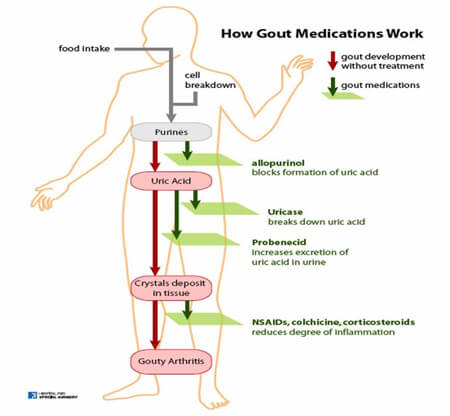
Double action of Allopurinol with Probenecid
I have gout(diagnosed) since 1978. I use colchicine when experiencing flares. I have tried herbal /natural remedies without success. I finally went onto Allopurinol after viewing articles from your website Keith. I commenced at 100mg in April 2015 with urate level of 0.47mmol/L. My Urate level lowered to 0.40 and increasing Allopurinol to 150 mg resulted in urate of 0.37 3months later. However inceasing Allpurinol to 200mg didn’t result in any change to urate which remained at 0.37mmol/L in December 2015. My GP is reluctant to suggest any increase in Allopurinol as it felt my urate level has “plateaued and any increase is not advisable.
I also have chronic gout in my left second toe top joint which has leaked tophi with an open wound for about the last 2 years. There has been no noticeable improvement to this joint.
My GP has proposed I go onto a complimentary regime of Allopurinol (200mg) together with Probenicid – dosage unspecified, to reduce the joint tophi. He has had some success in another patient who has bad tophi (knobbly) in elbow and other joints.
My question is do other members have any experience of such dual medication and can offer any comment please?-
January 10, 2016 at 7:11 am #771
 Keith TaylorParticipant
Keith TaylorParticipantHi Neil, that’s a very interesting question about supporting allopurinol with probenecid (often sold under the Probalan brand). Allopurinol works by reducing the amount of uric acid our bodies produce. Probenecid works by encouraging our kidneys to excrete more uric acid in our urine.
Before I comment further, I must apologize, Neil. You originally submitted your question via my Gout Helpdesk (aka the orange Gout Help button). I have to admit I’ve been overwhelmed by the number of tickets in the helpdesk. I’m slowly working through them, but I always give priority to GoutPal members who post directly in the forums. I’ll mark your Helpdesk ticket as ‘Resolved’ and continue to help you in this forum.
Back to allopurinol with probenecid. This is a good idea for some patients, and if your doctor wants to try it, then it’s a good idea if it lowers your uric acid. Having said that, personally, I would ask for another allopurinol increase first.
The reason I say that is because to describe the level as “plateaued” based on one result seems premature to me. This is especially true when you have a significant burden of uric acid crystals. Blood tests only measure dissolved urate. So, if a large number of crystals start to dissolve, blood test results will show slightly higher levels. Your test results went from 0.40 to 0.37 with 150 mg allopurinol daily. This is a 7.5% fall. When I’m thinking about uric acid, I regard the uric acid range as more significant than an individual test result. In essence, any single test result can easily fluctuate by 10% from natural daily fluctuations, dissolving crystals, or both. I believe this is a possible explanation for your static uric acid level.
I’ve seen other cases of allopurinol being supported by probenecid. From memory, these have involved higher allopurinol doses, and static results over more than one increase.
Ultimately, it’s always best to discuss the pros and cons with your doctor and reach a mutually agreed strategy. There are other factors that your doctor might be aware of. Significantly, there might be reasons why he is reluctant to increase allopurinol beyond a relatively low dose. I always recommend that anyone taking any uric acid lowering treatment should combine uric acid blood tests with kidney function and liver function tests. It might be that the results of these persuade your doctor against increasing allopurinol further.
It’s great that your doctor realizes the need to get uric acid lower. It is definitely your best chance of reducing your urate burden, which will shrink your tophi.
I think you have to check that there are no special reasons for restricting your allopurinol dose. Then, the question is if it’s better to increase allopurinol, introduce probenecid, or both. That’s the discussion you need with your doctor.
I hope this helps. If not, please ask for clarification. Otherwise, I look forward to reading the outcome of your visit.
-
January 10, 2016 at 7:21 am #772
 Keith TaylorParticipant
Keith TaylorParticipantBy the way, Neil, I should have asked about your fluid intake. Are you adequately hydrated? That means urine should be pale straw colored. Dehydration can restrict uric acid excretion.
-
January 10, 2016 at 12:33 pm #774
Anonymous
InactiveHi Keith
Thanks – I see the ticket is “Resolved”. I keep fairly well hydrated (urine coour seems Ok)- I try to be reasonably disciplined in keepng up my daily water intake. My initial thought was to icrease Allopurinol to 250mg and then get another blood, kidney and liver function test in a month or so. After reading your comments I will see my GP this week and see what we can agree to. I really would prefer not to complicate my medication regime unless there really is no other option – will keep you posted -
January 12, 2016 at 9:51 am #788
 Keith TaylorParticipant
Keith TaylorParticipantThanks Neil, that sounds sensible to me.
My only other comment would be that it seems a long time between each of your earlier blood test. It takes two weeks for allopurinol to reach it’s full effect, so that is the minimum time between tests. Anything beyond six weeks seems like missed opportunity to me. Maybe you can make future appointments monthly until you’ve got uric acid well below 0.30mmol/L.
Anyway, I look forward to your next report.
-
May 21, 2016 at 5:48 pm #1159
 Keith TaylorParticipant
Keith TaylorParticipant“The new GP is not a fan of blood tests and believes in bog standard 300mg dose Allopurinil to fix gout.” That’s madness. A serious breach of the Hippocratic Oath!
Anyway, it sounds like you are managing OK despite him. Certainly, at 0.33 you should be debulking uric acid crystals slowly. For USA readers, 0.33mmol/L uric acid converts to 5.55mg/dL.
Neil, it’s terrible news about the plans to introduce blood test charges in Oz. Blood tests are vital for safe gout management. I’d go so far to say, it’s a lottery without the test. All gout sufferers need to know accurate uric acid levels. But, everybody on the planet needs to know liver function and kidney function is OK.
Only this morning, I was thinking about ways I might help needymeds.org raise awareness and funding. Do you know if there is anything similar in Australia, Neil?
And to readers from other countries, what is the situation where you live? In the UK, testing is free to everyone regardless of income. I think this is a basic human right that everyone on the planet should have.
Anyway, Neil, this topic is about you, so I’m pleased to see you are recovering. I can’t wait to see you go 6 months without a flare.
Keith
Unresolved Support Requests
When you are happy that the problems you have raised have been resolved, please change the status of your topic.
You have to log in first. Once you are logged in, you will see a dropdown at the top of your first post. Change it fromNot ResolvedtoResolved. There’s nothing else to click. There’s no need to post any additional information, unless you want to.
Changing the status does not stop you from adding information later. It just lets me know that your problem is no longer urgent. If your problem becomes urgent again, you can change status back again.
-
-
January 28, 2016 at 6:16 pm #893
Gout Patient
ParticipantBecause of hair loss from allopurinol, my rheumy decreased my allopurinol dosage and made up the difference with probenecid. As a result I’m now having my first flare in six months. Is anyone else on this combination therapy? Is it less effective than a higher dose of allopurinol?
-
February 2, 2016 at 10:24 am #918
 Keith TaylorParticipant
Keith TaylorParticipantI’ve discussed the combination of allopurinol and probenecid with other gout sufferers. It’s a great combination for some gout patients. There are some important factors to consider, but before I ask about those, there is a much more vital question I have to ask:
What are your uric acid levels?
Have you have had a gout flare soon after changing your gout medications? It is much more likely to be a sign that your treatment is working better. But, I don’t want to waste your time discussing percentages. Please post your latest uric acid test results. That is most important. If you have time, I can also help you better with more information about:
How long have you had gout?
When did you start allopurinol?
History of allopurinol doses
History of gout flaresIn general Linda, the more information you can give me about your gout history, the better I can help you.
Probenecid with allopurinol can be a lifesaver or a waste of time. It depends on you.
-
February 2, 2016 at 12:32 pm #926
 Keith TaylorParticipant
Keith TaylorParticipantAnd, Linda
Since I wrote that, I’ve spotted you’ve joined in with some other topics here on the gout forum. That’s really good news for me. We all learn so much more when the discussions have different points of view, and different experiences.
Thank you Linda. I can’t wait for your latest test results. I can see from Robert’s topic about tendinitis that you had uric acid of 10.9 at one point. I wonder when that was, and how much it has fallen since then?
-
February 2, 2016 at 5:08 pm #932
Gout Patient
ParticipantKeith: I was diagnosed with gout in June of last year, with a UA of 10.9, sed rate 79. DIP joint in my hand, but in retrospect, I probably had at least two flares earlier. One in the classic big toe maybe six years ago, one in a foot a year later following surgery on the other big toe,x and in a knee one year ago. Started allopurinol in June, last UA was 6.0 in December. My rheumy targets 6.0 and doesn’t feel the side effects of most medications warrant shooting for 4 type levels. As I get an annoying skin rash from allopurinol, I concur. Started at 50mg/day, then 100, then 150, then up to 200 by late August. UA at that time was 7.9.
I had a lot of flares over the past summer as I ramped up the allopurinol. Right ankle/foot three times, left ankle/foot once. Treated with 30mg Predisone for a week, then taper. Relief was considerable in every case after about 5 hours. Just had a flare last week in a middle toe, but it was relatively minimal. This was the first flare since August, so I was ‘flare-free’ for 5 months on allopurinol. I take 400mg of Celebrex daily for OA, and that was enough for my toe so I could walk; didn’t need Predisone.. I can’t take colchicine..GI symptoms are horrible.
Almost forgot..started probenecid 1/2 tab at the beginning of January, ramped up to one tab after two weeks. The toe flare occurred after I was taking the combined allopurinol 100 mg, probenecid one tab for two weeks. My worry is that the action of probenecid isn’t enough to stay ahead of my production of purines.I wouldn’t have changed medications except that I’ve lost half my hair since I started on allopurinol last July. It’s a known side effect, but still rare. Lucky me…
-
February 9, 2016 at 1:29 pm #963
 Keith TaylorParticipant
Keith TaylorParticipantLinda, thanks for the extra info.
Getting that flare after two weeks of changing meds can be one of two things:
1. It would’ve happened anyway.
2. It’s a result of uric acid falling, and more partially dissolved uric acid crystals waking up the immune system.The only way to know is from your uric acid test results. Increased uric acid takes months to cause a flare. Decreased uric acid might cause one sooner because of the aforementioned partially dissolved crystals. Until your uric acid burden is dissolved, you run a risk of gout flares. There’s very little you can do about that except to go as low as possible to shorten the risk period.
-
February 9, 2016 at 2:35 pm #969
Gout Patient
ParticipantJust had a new UA and it’s 4.0! I am thrilled. Went out and had a little steak 🙂 Bad, I know, but it’s been so long and I think I have a cushion now. My doc is thinking of moving me completely to Probenecid as it worked faster in bringing down my levels, doesn’t cause a rash, and hopefully won’t make more of my hair fall out!!! I guess I am an undersecreter more than an over producer. Or both..who knows?
Am having other orthopedic problems now and am up to 40mg prednisone daily. He’s sending me for MRIs on Friday to see if the current problem is mechanical or inflammatory. All my lab work is remarkable in its ‘unremarkableness’, unfortunately. But, with all the sterioids, I feel fantastic! Too bad I have to start tapering….
-
February 16, 2016 at 1:16 pm #981
 Keith TaylorParticipant
Keith TaylorParticipantGreat news on the uric acid test, Linda! Let’s hope it’s the start of much less pain for you. If you have other causes of joint pain, solving your gout won’t make that better. But overall, you are bound to feel better.
I think that’s a great reason for celebration. Completely in keeping with my new philosophy of ‘meat as a treat’ 🙂
As it sounds like you’re an under-excreter of uric acid, a glass or two of skim milk will probably counteract any increase from a small steak. (Disclaimer: that is a guess, not scientific analysis)
-
-
July 10, 2016 at 7:33 pm #1415
GoutPal Victim
ParticipantI’m 69 with a heart condition (diuretics, beta blockers, low EF, etc). In the last year, I’ve had my first and only two “minor” (?) flairs of gout. Somewhat uncomfortable, but I could still walk, etc. Absolutely nothing like the one time I had kidney stones. Straight Colchicine seems to have resolved both issues after (only?) 3 doses. My uric acid level is 9.1. I don’t eat organ meat, but do like shrimp and probably over use bourbon. Beer and wine I can usually pass on although I think my ‘second bout’ of gout was a result of one night with too much merlot. Saw my GP last week. He ordered Colchicine-Probenecid twice a day basically for the rest of my life. My Medicare Rx insurer just somehow automatically sent me a 90 day supply. And charged my credit card $175 freakin dollars!!!
So why didn’t I get, if anything, Allopurinol which is $14 a month without insurance at Walmart? Maybe if I’m really need to be cautious, I need more of a gout specialist than my GP. Any suggestions on a specialist? Anyone interested in some fresh, factory sealed Colchicine-Probenecid tablets (500-.5MG Tab)?
-
July 15, 2016 at 8:23 am #1422
 Keith TaylorParticipant
Keith TaylorParticipantHi Gary,
I think your doctor is right to take this seriously. 9.1 is far too high for uric acid.
Even though you can manage occasional pain now, it’s going to get worse. Untreated high uric acid means that crystals are developing in your body every day.
Some days, your immune system deals with uric acid crystals without you noticing. Other days, you get symptoms that range from a little itching or discomfort, through to full-blown gouty agony. It gets worse after that, as joints start to crumble. It’s especially bad if your prone to kidney stones. Untreated gout leads to kidney damage. And, skin and heart are other common targets. All organs apart from the brain are at risk.
I wanted to mention all that to underline the dangers. Also, to point out that your second gout attack was nothing to do with red wine. It was caused by crystals that started to grow many months, or years, ago.
But, your main question is about choice of treatment.
Probenecid is usually prescribed for patients who have low uric acid excretion rates. This is tested by measuring the amount of uric acid in urine over a 24-hour period. Have you had that test?
Allopurinol is best targeted at over-producers. However, it can be effective for some under-excreters as well. So, many doctors try allopurinol first. Then, they might introduce probenecid if allopurinol isn’t getting uric acid low enough.
After 6 months of safe uric acid levels, you definitely do not need colchicine.
If you’ve lost confidence in your GP, I think it’s best to see a rheumatologist. I guess it depends how easy it is for you to see one. Also, we might get to understand your GP’s reasoning better if we know about the urine test I mentioned.
It comes down to whatever you think is best for you.
-
-
March 2, 2017 at 9:46 am #2700
 Keith TaylorParticipant
Keith TaylorParticipantIs it safe for him to take any indomethacin while on the probenecid?
I see no reason why not. But, the indomethacin dose for gout should be prescribed by your doctor. Maximum dose is usually required for gout pain. And, your doctor and pharmacist need to check it is compatible with all medications and supplements that your husband is taking.Does he take the colchicine only during flares?
Colchicine is best taken as a preventative before flares start. Or, take it at the very first sign of a flare. Once the gout flare starts, colchicine doesn’t do anything to reduce the pain. It just stops inflammation getting worse, until nature, or anti-inflammatories do their work.I read to drink baking soda water while on the probencid
You need to stop reading Baking Soda Gout Myths!how much should he take of the baking soda?
None! Because Baking Soda for Gout is Dangerous.Is probenecid safer or more dangerous than allopurinol?
Both are safe. Allopurinol has a genetic risk for some Han Chinese, Thai, and Korean gout sufferers. But, that can be screened for. One danger of probenecid is that it might not get uric acid low enough to be safe. You should be able to check that at his next blood test.The real danger is excess uric acid. Gout pain in the joints is best seen as a warning sign. The warning is for a progression of effects of uric acid crystals. These get increasingly dangerous:
- Permanent joint damage.
- Visible tophi (lumps of uric acid crystals) that damage the skin.
- Tophi spread to all organs, except the brain. Kidney failure or heart failure are the usual causes of death from gout.
Maybe you husband should look at some of my tophi pictures. Who on earth wants to spend their later years suffering like that? And, that’s really the point that your husband has to understand. It’s very easy in your thirties and forties to shrug off gout with a painkiller or two. But gout always gets worse when uric acid is above 5mg/dL. The longterm effects that I listed get worse every day – even when there is no pain. So, at a time of life when he is less able to cope, your husband will have to fight much bigger and more painful problems.
I do understand how your husband feels. I put off going on allopurinol for far too long. Even when I started to understand the real longterm dangers. Eventually, when I couldn’t tell the difference between gout and a broken knee, I took the plunge. It’s really great knowing that I do not have to face a gout flare ever again.
With the right pain control package, there is no need to suffer during the time it takes to get rid of old crystals. I hope I can help your husband to take control of his gout properly. Before it’s too late.
-
May 21, 2016 at 8:03 am #1158
Anonymous
InactiveHi Keith
Sorry I did not reply as I have had a complicated time recently with other health concerns from gout including chest infection, skin problems etc. and a change of GP because my original one went on extended leave.
The new GP is not a fan of blood tests and believes in bog standard 300mg dose Allopurinil to fix gout. However he did fix my leaky DIP joint second left toe with solid course of antibiotics (Test indicated Staph infection) The skin is slowly healing over what used to be a big scab although the joint is still quite pink – probably tophi underneath!!
Regarding the Gout/ urate levels I increased Allopurinol to 250mg on 2/2/16 and had a blood test on 18/4/16 with reading of 0.33mmol/L. This is the lowest ever !!! – down from 0.37 in 12/15. I only got this test because I had a full blood test for my fungal chest infection!
My current GP does not believe urate levels relate to tophi production and also with Government budget cuts to pathology testing(currently free but from July cost for patient) I am unsure of when I will have the next blood test.
At this stage I will stay on 250mg Allopurinol alone and see my original GP when shereturns from leave and see what she thinks of my situation. I have not had a flare since just a few days after I increased to 250mg early February.
Thanks for your website and the help it has been for me
Regards
Neil Woodward
-
-
AuthorPosts
The forum ‘Help My Gout! The Gout Forum’ is closed to new topics and replies.